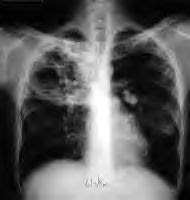
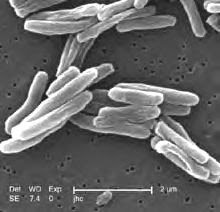
Extensively drug resistant tuberculosis (XDR-TB) represents a spectre for the civil society and a major challenge for the TB control community. In this issue, the TBNET study reports on 4,583 confirmed TB cases in Italy, Germany, Estonia and Russia (Archangels Oblast). Treatment outcomes of 64 XDR (1) cases, 267 multidrug-resistant (MDR) (2) cases resistant to all first-line drugs, and of 94 "other" MDR cases (susceptible, at least, to one first-line anti-TB drug) are compared. The results of the study demonstrate that XDR cases have a worse outcome (death or failure, i.e. treatment fails to render the patient non-infectious) than MDR cases resistant to all first-line drugs, and of "other" MDR cases (susceptible, at least, to one first-line anti-TB drug). The study also demonstrates that the XDR definition proposed by WHO has both a clinical (predicts poor outcome), and operational value (confirming these cases are resistant to both first-line drugs and key second-line ones).
(1) XDR: cases resistant at least to isoniazid and rifampicin, plus at least one fluoroquinolone (new generation second-line drug) and one injectable second-line drug(2) MDR: cases resistant to at least isoniazid and rifampicin, the two most powerful anti-TB
http://tinyurl.com/2e9ogm
WHAT'S NEW IN TUBERCULOSIS
Sunday, 30 September 2007
Offering Choice To Tuberculosis Patients Improves Treatment Outcomes
Tuberculosis (TB) is an important disease. More than a third of the world's population has been infected with the disease. Given the right conditions, these infections can progress from latent to active disease. Even in Europe, TB is increasing in several countries. If latent TB infection is treated effectively, then many individuals can be prevented from developing TB and passing it on to their friends and families before they realise they are ill. This study, undertaken by Timothy Rennie (NE London TB Network, Homerton University Hospital, London, UK) and his colleagues, shows that giving the choice of treatment for latent infection (either a three- or a six-month course) improves adherence to therapy. More patients taking the three-month course completed treatment (60%) than those taking the six-month course (46%). Patients generally preferred the shorter three-month course. Child patients were more likely to complete treatment and patients who missed clinics before starting treatment were less likely to complete therapy. Just under one in 18 patients had the therapy stopped because of side effects, but there was no difference in side effects between the different courses of treatment. TB still needs long courses of antibiotics compared with other bacterial infections. Simple measures, such as offering choice, can be very effective. Safe, short regimens are likely to be preferred by patients and greater efforts should be made to identify these
http://tinyurl.com/2vyaba
http://tinyurl.com/2vyaba
Tuesday, 25 September 2007
Money for research - Gates' Foundation
The Bill and Melinda Gates Foundation announced a new package of funding, 18 September, to accelerate and build on existing technologies to combat tuberculosis (TB).
The US$280 million grant is the largest single donation for TB research and development by the foundation, which aims to donate US$900 million to research by 2015.
The grants will be used for vaccine development (US$200 million), developing diagnostic tests (US$62 million) and drug discovery (US$18 million).
Tachi Yamada, president of the Gates Foundation Global Health Program, told a press briefing that the diagnostic test for TB —— sputum smear microscopy —— is one hundred years old and fails to diagnose half of all cases in developing countries.
Yamada also said that the only TB vaccine, known as the BCG, is over 80 years old and rarely effective after childhood, while existing TB drugs are becoming less effective as resistance to them grows.
New, effective vaccines could save 30 million lives by 2030, said Jerald Sadoff, president of Aeras Global TB Vaccine Foundation, whose company is receiving the US$200 million over five years to take six newly-identified TB vaccine candidates into clinical trials.
The South African Tuberculosis Vaccine Initiative will work with Aeras to implement the trials. The Initiative's clinical director, Tony Hawkridge, highlighted the critical role of scientists in Africa and other developing countries, saying they had been "at the forefront of the basic science underpinning vaccinology".
The Switzerland-based non-profit organisation Foundation for Innovative New Diagnostics (FIND) will receive US$62 million to develop rapid, point of care TB diagnostic tests for developing countries.
Giorgio Roscigno, chief executive officer of FIND, said that they already had ten new diagnostic technologies in development, and hoped to gain WHO approval for at least three of them in the next five years.
Peter Small, senior program officer for TB at the Gates Foundation, said he hoped that pharmaceutical companies would take notice of the grants for drug development. He said that one of the reasons that TB drugs have not kept up with changing situations —— such as drug resistance —— is that in the last 50 years "no one has really tried".
Http://tinyu;.com/3dfgtz
The US$280 million grant is the largest single donation for TB research and development by the foundation, which aims to donate US$900 million to research by 2015.
The grants will be used for vaccine development (US$200 million), developing diagnostic tests (US$62 million) and drug discovery (US$18 million).
Tachi Yamada, president of the Gates Foundation Global Health Program, told a press briefing that the diagnostic test for TB —— sputum smear microscopy —— is one hundred years old and fails to diagnose half of all cases in developing countries.
Yamada also said that the only TB vaccine, known as the BCG, is over 80 years old and rarely effective after childhood, while existing TB drugs are becoming less effective as resistance to them grows.
New, effective vaccines could save 30 million lives by 2030, said Jerald Sadoff, president of Aeras Global TB Vaccine Foundation, whose company is receiving the US$200 million over five years to take six newly-identified TB vaccine candidates into clinical trials.
The South African Tuberculosis Vaccine Initiative will work with Aeras to implement the trials. The Initiative's clinical director, Tony Hawkridge, highlighted the critical role of scientists in Africa and other developing countries, saying they had been "at the forefront of the basic science underpinning vaccinology".
The Switzerland-based non-profit organisation Foundation for Innovative New Diagnostics (FIND) will receive US$62 million to develop rapid, point of care TB diagnostic tests for developing countries.
Giorgio Roscigno, chief executive officer of FIND, said that they already had ten new diagnostic technologies in development, and hoped to gain WHO approval for at least three of them in the next five years.
Peter Small, senior program officer for TB at the Gates Foundation, said he hoped that pharmaceutical companies would take notice of the grants for drug development. He said that one of the reasons that TB drugs have not kept up with changing situations —— such as drug resistance —— is that in the last 50 years "no one has really tried".
Http://tinyu;.com/3dfgtz
Friday, 21 September 2007
Moxifloxacin vs Isoniazid
Moxifloxacin performed as well as isoniazid in treating pulmonary tuberculosis (TB) in a multinational phase. Subjects were randomized to receive 400 mg/day of moxifloxacin or 300 mg/day isoniazid, given 5 days per week for 8 weeks. All patients also were treated with rifampin, ethambutol and pyrazinamide on the same schedule. The primary measure of treatment success was two consecutive sputum cultures negative for TB organisms. Time to first negative culture was a secondary endpoint. Based on earlier clinical studies, the investigators were hoping to see a treatment success rate of 88% among moxifloxacin patients completing the study protocol. The differences between drugs were not significant.
http://tinyurl.com/2s8qv
http://tinyurl.com/2s8qv
Anthropo-zoonotic transfer of tubercle bacillus
Human tuberculosis caused the partial paralysis in the young baboon, Marcus, that was put down in June. But TB experts have warned that, rather than baboons being viewed as a health threat to humans, the diagnosis should sound the alarm about the transfer of human disease to wild animals. It was initially feared that Marcus, a research baboon, had been poisoned and a battery of tests were performed to determine the cause of his paralysis and eventual death.
Revealing the news of Marcus's autopsy results, the multirepresentative Baboon Management team's Esme Beamish said they were concerned about the appearance of human TB in a baboon. Paul van Helden, professor of medical biochemistry at Stellenbosch University and a TB expert, said human disease was transferred to wild animals through close contact with them and inappropriate management of refuse. Beamish said the Peninsula's baboon population of 384 180 was already stressed due to isolation, ring fencing by urbanisation and conflict with humans. "A health risk introduced by humans is a serious threat to their continued presence in the Peninsula," she warned.
http://tinyurl.com/2835ft
Revealing the news of Marcus's autopsy results, the multirepresentative Baboon Management team's Esme Beamish said they were concerned about the appearance of human TB in a baboon. Paul van Helden, professor of medical biochemistry at Stellenbosch University and a TB expert, said human disease was transferred to wild animals through close contact with them and inappropriate management of refuse. Beamish said the Peninsula's baboon population of 384 180 was already stressed due to isolation, ring fencing by urbanisation and conflict with humans. "A health risk introduced by humans is a serious threat to their continued presence in the Peninsula," she warned.
http://tinyurl.com/2835ft
More on Moxifloxacin; and good news for mice!
A team of Brazilian and US TB experts reported at a meeting of the American Society for Microbiology that adding the drug moxifloxacin to a standard cocktail of antibiotics increased by 17 percent the number of patients who cleared active TB infection from their lungs, from 68 to 85 percent. The drug mixture shortened by two months the time needed to cure the dreaded lung ailment which kills some 1.5 million people each year, mostly in developing countries, experts reported at a meeting of the 47th Interscience Conference on Antimicrobial Agents and Chemotherapy (ICAAC).
The new combination drug therapy uses moxifloxacin in the place of an older, more traditional anti-TB drug, ethambutol.
"This is the most compelling evidence in nearly 25 years that a novel antibiotic drug combination works better than the current gold standard at curing active TB infection," said study senior author Richard Chaisson, a professor of medicine, epidemiology and international health at The Johns Hopkins University School of Medicine.
"Beyond the obvious value of healing patients more quickly, a shorter treatment time could also cut down on transmission of the disease to others and make it easier for health care workers worldwide, who are overwhelmed by large numbers of patients, to treat more people and to treat them faster" said Chaisson, who also heads Hopkins's Center for Tuberculosis Research. He noted nearly nine million new cases of TB are diagnosed each year in the world, and more than one-and-a-half million people die from the disease.
"Better vaccines, diagnostics, and drugs could dramatically improve the fight against TB, especially in poor countries where large numbers of people are affected by the disease," said Peter Small, senior program officer for Tuberculosis at the Gates Foundation.
Another study on mice performed by Johns Hopkins researchers and released at the conference found that replacing the antibiotics rifampin and isoniazide with moxifloxacin and rifapentine allow lab mice to get over TB in 10 weeks rather than six months
http://tinyurl.com/2f3a9a
The new combination drug therapy uses moxifloxacin in the place of an older, more traditional anti-TB drug, ethambutol.
"This is the most compelling evidence in nearly 25 years that a novel antibiotic drug combination works better than the current gold standard at curing active TB infection," said study senior author Richard Chaisson, a professor of medicine, epidemiology and international health at The Johns Hopkins University School of Medicine.
"Beyond the obvious value of healing patients more quickly, a shorter treatment time could also cut down on transmission of the disease to others and make it easier for health care workers worldwide, who are overwhelmed by large numbers of patients, to treat more people and to treat them faster" said Chaisson, who also heads Hopkins's Center for Tuberculosis Research. He noted nearly nine million new cases of TB are diagnosed each year in the world, and more than one-and-a-half million people die from the disease.
"Better vaccines, diagnostics, and drugs could dramatically improve the fight against TB, especially in poor countries where large numbers of people are affected by the disease," said Peter Small, senior program officer for Tuberculosis at the Gates Foundation.
Another study on mice performed by Johns Hopkins researchers and released at the conference found that replacing the antibiotics rifampin and isoniazide with moxifloxacin and rifapentine allow lab mice to get over TB in 10 weeks rather than six months
http://tinyurl.com/2f3a9a
NEW DRUG FOR TB
Bayer AG's Avelox, set to become the first new type of medicine for tuberculosis in 30 years, may shorten treatment time by two months and slow the development of deadly, drug-resistant strains. Combining the antibiotic with three other therapies might cure the disease in four months instead of six, according to research funded by the Gates Foundation and the U.S. government. As a result, the number of patients who stop treatment too early may fall, slowing the spread of a disease that infects about 2 billion people, scientists say.
TB approval for Avelox, already used to treat pneumonia, may help contain lethal multidrug-resistant TB, the germ carried by Atlanta lawyer Andrew Speaker when he boarded a flight to Paris in May. Doctors at an infectious disease meeting this week in Chicago will hear results of a clinical trial. The findings will be crucial to the drug's approval as early as 2011.
The chemical structure of the drug, also known by the generic name moxifloxacin, can attach to both fatty and watery molecules, allowing it to penetrate TB efficiently, he said.
The Seattle-based Gates Foundation, the world's largest charitable fund, has given $140 million to the Global Alliance to develop new TB drugs. Without that support and direction, along with funds from the U.S. Food and Drug Administration for trials of Avelox, new TB drugs would never get approval, public researchers said. The market is small and treatment trials are so expensive and lengthy that most companies won't touch them.
Most patients carry TB in a dormant, non-infectious form. Even when active, the germ grows slowly, dividing about once a day, compared with other bacteria that might replicate every 20 minutes. The plodding pace gives antibiotics few opportunities for bacterial sabotage, and the organism also has a fatty outer coat that keeps most drugs out entirely.
Multi-drug resistant TB affects about 400,000 people worldwide. Speaker, the lawyer who put hundreds of airline travelers at risk of exposure by taking transatlantic flights, underwent surgery in a Denver hospital to remove infected tissue. Public health officials have spent decades trying to find the best ways to make sure TB patients finish their typical six- month treatments, which once lasted at least 18 months. Skipping doses allows resistant strains to thrive and spread to other people, said David Ashkin, the tuberculosis controller for Florida. Ashkin confines dozens of TB patients to a secure hospital in Lantana annually to make sure they take all their drugs and don't spread germs.
`Six months of therapy is very hard for some patients, with a shorter regimen, more people might complete therapy.'' About a third of patients drop out in the final two months of treatment, the TB alliance's Spigelman said. His group will use Gates Foundation support to begin testing four-month treatment with the Bayer drug later this year. He plans eventually to test whether other drug combinations can beat TB in three months or even two.
http://tinyurl.com/2v5lcn
TB approval for Avelox, already used to treat pneumonia, may help contain lethal multidrug-resistant TB, the germ carried by Atlanta lawyer Andrew Speaker when he boarded a flight to Paris in May. Doctors at an infectious disease meeting this week in Chicago will hear results of a clinical trial. The findings will be crucial to the drug's approval as early as 2011.
The chemical structure of the drug, also known by the generic name moxifloxacin, can attach to both fatty and watery molecules, allowing it to penetrate TB efficiently, he said.
The Seattle-based Gates Foundation, the world's largest charitable fund, has given $140 million to the Global Alliance to develop new TB drugs. Without that support and direction, along with funds from the U.S. Food and Drug Administration for trials of Avelox, new TB drugs would never get approval, public researchers said. The market is small and treatment trials are so expensive and lengthy that most companies won't touch them.
Most patients carry TB in a dormant, non-infectious form. Even when active, the germ grows slowly, dividing about once a day, compared with other bacteria that might replicate every 20 minutes. The plodding pace gives antibiotics few opportunities for bacterial sabotage, and the organism also has a fatty outer coat that keeps most drugs out entirely.
Multi-drug resistant TB affects about 400,000 people worldwide. Speaker, the lawyer who put hundreds of airline travelers at risk of exposure by taking transatlantic flights, underwent surgery in a Denver hospital to remove infected tissue. Public health officials have spent decades trying to find the best ways to make sure TB patients finish their typical six- month treatments, which once lasted at least 18 months. Skipping doses allows resistant strains to thrive and spread to other people, said David Ashkin, the tuberculosis controller for Florida. Ashkin confines dozens of TB patients to a secure hospital in Lantana annually to make sure they take all their drugs and don't spread germs.
`Six months of therapy is very hard for some patients, with a shorter regimen, more people might complete therapy.'' About a third of patients drop out in the final two months of treatment, the TB alliance's Spigelman said. His group will use Gates Foundation support to begin testing four-month treatment with the Bayer drug later this year. He plans eventually to test whether other drug combinations can beat TB in three months or even two.
http://tinyurl.com/2v5lcn
Saturday, 15 September 2007
Treatment of TB in Rural China
China's healthcare system has been swept up in the country's tide of capitalism, and it is the rural poor who are paying the price
The richest man in one of the poorest villages in China is the "barefoot doctor" Hua Wanxiang, who sells cigarettes, beer and antibiotics. It was an easy move. The only medical equipment he owns is a stethoscope, some tweezers and a sterilising bowl. He can now sell tobacco while referring locals to hospital for lung diseases; flog crates of beer one day and painkillers the next.
This shift from public service to market principles is entirely in keeping with the wider transformation of healthcare in China, which is now among the most market-driven in the world. Surveys suggest that health problems account for between a third and a half of all cases of destitution. The health ministry says three-quarters of the rural patients who declined to undergo recommended hospital treatment did so because they could not afford it.
A peasant saying has it that a pig must be taken to market every time an ambulance siren wails, a year's work is ruined as soon as you sleep in a hospital bed, and if you are struck with a serious disease, 10 years of savings go up in smoke. For Mo Wangfa, the cost of contracting spinal tuberculosis has been even higher. Since 1999, the farmer has spent more than 10,000 yuan on check-ups and treatment. With no support from the government and no insurance, he had to borrow most the money, much of it from loan sharks who charge 6% interest. What passes for family treasures now are his x-ray charts and medical reports, all of which cost far more than he could ever earn. He is still too sick to work his fields. "Before the illness, I was doing reasonably well. I wasn't rich, but I wasn't poor. Now I have big debts," he says. "I plan to ask my children to go the cities to find work so we can pay back the money."
Aside from compassion, doctors have few incentives to reduce costs or pursue long-term public health goals. In some areas, tuberculosis and other preventable diseases are making a comeback because vaccination programmes are under-funded. Meanwhile, the privatisation of medicine is blamed for the rampant over-prescription of drugs, which has created new strains of TB and other diseases that are resistant to antibiotics.
Sarah Boseley
http://www.guardian.co.uk/china/story/0,,2168522,00.html
The richest man in one of the poorest villages in China is the "barefoot doctor" Hua Wanxiang, who sells cigarettes, beer and antibiotics. It was an easy move. The only medical equipment he owns is a stethoscope, some tweezers and a sterilising bowl. He can now sell tobacco while referring locals to hospital for lung diseases; flog crates of beer one day and painkillers the next.
This shift from public service to market principles is entirely in keeping with the wider transformation of healthcare in China, which is now among the most market-driven in the world. Surveys suggest that health problems account for between a third and a half of all cases of destitution. The health ministry says three-quarters of the rural patients who declined to undergo recommended hospital treatment did so because they could not afford it.
A peasant saying has it that a pig must be taken to market every time an ambulance siren wails, a year's work is ruined as soon as you sleep in a hospital bed, and if you are struck with a serious disease, 10 years of savings go up in smoke. For Mo Wangfa, the cost of contracting spinal tuberculosis has been even higher. Since 1999, the farmer has spent more than 10,000 yuan on check-ups and treatment. With no support from the government and no insurance, he had to borrow most the money, much of it from loan sharks who charge 6% interest. What passes for family treasures now are his x-ray charts and medical reports, all of which cost far more than he could ever earn. He is still too sick to work his fields. "Before the illness, I was doing reasonably well. I wasn't rich, but I wasn't poor. Now I have big debts," he says. "I plan to ask my children to go the cities to find work so we can pay back the money."
Aside from compassion, doctors have few incentives to reduce costs or pursue long-term public health goals. In some areas, tuberculosis and other preventable diseases are making a comeback because vaccination programmes are under-funded. Meanwhile, the privatisation of medicine is blamed for the rampant over-prescription of drugs, which has created new strains of TB and other diseases that are resistant to antibiotics.
Sarah Boseley
http://www.guardian.co.uk/china/story/0,,2168522,00.html
Friday, 14 September 2007
Bovine TB in Elk
Officials from Riding Mountain National Park say just three of more than a thousand elk and deer tested have bovine tuberculosis.
During the winter and spring of 2007, 128 elk were captured and blood tested as part of the park’’s surveillance and monitoring program. Three of these animals tested positive for bovine TB on culture. The animals were captured from a helicopter using a net fired from a netgun, a blood sample was taken, and then were released wearing collars for research and tracking purposes.
Manitoba Conservation, in co-operation with Parks Canada and Manitoba Agriculture, Food, and Rural Initiatives, also continued its surveillance of hunter-killed elk and deer continued during the 2006-07 hunting seasons. Approximately 950 elk and deer samples were collected from hunters and then examined at the Riding Mountain National Park lab.
None of these animals tested positive for bovine TB.
http://www.winnipegfreepress.com/breakingnews/local/story/4038307p_4647487c.html
During the winter and spring of 2007, 128 elk were captured and blood tested as part of the park’’s surveillance and monitoring program. Three of these animals tested positive for bovine TB on culture. The animals were captured from a helicopter using a net fired from a netgun, a blood sample was taken, and then were released wearing collars for research and tracking purposes.
Manitoba Conservation, in co-operation with Parks Canada and Manitoba Agriculture, Food, and Rural Initiatives, also continued its surveillance of hunter-killed elk and deer continued during the 2006-07 hunting seasons. Approximately 950 elk and deer samples were collected from hunters and then examined at the Riding Mountain National Park lab.
None of these animals tested positive for bovine TB.
http://www.winnipegfreepress.com/breakingnews/local/story/4038307p_4647487c.html
More efforts on drugs for orphan diseases
A group of leading drug researchers today announced the formation of a non-profit international institute to channel top talent and drug candidates from the world’’s leading research labs into a major, new global assault on tuberculosis (TB), malaria, and HIV/AIDS.
Founders of the International Drug Discovery Institute (iDDi) (www.i-ddi.org) hope to fill a gap in commercial drug development that has left large populations in developing nations exposed to epidemic diseases with no new or affordable cures. In effect, iDDi’’s innovative model seeks to skirt barriers that have hampered the development of new therapeutic agents for scourges like malaria or TB for the past 40 years.
""Through my long career in drug discovery, I have found it incredibly frustrating that every year, millions of human beings still perish from diseases that could and should be curable,"" said Dr. Alan Kozikowski, founder and chief science officer of iDDi. ""We know that the world’’s best scientific minds –– collaborating on promising, new drug candidates –– and empowered by new machine-based screening technologies, could launch a Manhattan-style project that would wipe these diseases from the face of the earth.""
Explained John McCall, an iDDi director and former vice president of drug development at Pharmacia & Upjohn, Inc., ""iDDi is the embodiment of this new approach to drug discovery and development. We will empower an innovative network of global scientific talent to break through organizational, national, and economic barriers to deliver new drugs more expeditiously to the people who need them.""
IDDi is being formed specifically to accelerate drug discovery and development for neglected and orphan diseases, and has already begun outreach to major philanthropic foundations with similar goals.
Its founders and collaborating scientists include research luminaries, such as Scott Franzblau, Ph.D., Director of the Institute for Tuberculosis Research at the University of Illinois at Chicago; Geoff Dow, Ph.D. a malaria researcher at the U.S. Army’’s Institute at Walter Reed Army Hospital; and Paul Wender, Ph.D., of Stanford University.
In addition to its technical resources, iDDi is developing a novel operational model aimed at making practical and affordable medicines available to those in need. To this end, Mohsen Marefat of The Althing Group has been retained to head the development and management of business operations for the Institute.
To date, iDDi has been funded by donations from angel benefactors. The Institute plans to launch an aggressive fundraising campaign to attract foundation support.
About iDDi
iDDi is a non-profit institute that will accelerate and streamline drug discovery by harnessing the power of technology and the expertise of select scientists, worldwide, to identify and bring to market effective and practical therapies for diseases afflicting millions. For more information, please visit www.i-ddi.org.
Founders of the International Drug Discovery Institute (iDDi) (www.i-ddi.org) hope to fill a gap in commercial drug development that has left large populations in developing nations exposed to epidemic diseases with no new or affordable cures. In effect, iDDi’’s innovative model seeks to skirt barriers that have hampered the development of new therapeutic agents for scourges like malaria or TB for the past 40 years.
""Through my long career in drug discovery, I have found it incredibly frustrating that every year, millions of human beings still perish from diseases that could and should be curable,"" said Dr. Alan Kozikowski, founder and chief science officer of iDDi. ""We know that the world’’s best scientific minds –– collaborating on promising, new drug candidates –– and empowered by new machine-based screening technologies, could launch a Manhattan-style project that would wipe these diseases from the face of the earth.""
Explained John McCall, an iDDi director and former vice president of drug development at Pharmacia & Upjohn, Inc., ""iDDi is the embodiment of this new approach to drug discovery and development. We will empower an innovative network of global scientific talent to break through organizational, national, and economic barriers to deliver new drugs more expeditiously to the people who need them.""
IDDi is being formed specifically to accelerate drug discovery and development for neglected and orphan diseases, and has already begun outreach to major philanthropic foundations with similar goals.
Its founders and collaborating scientists include research luminaries, such as Scott Franzblau, Ph.D., Director of the Institute for Tuberculosis Research at the University of Illinois at Chicago; Geoff Dow, Ph.D. a malaria researcher at the U.S. Army’’s Institute at Walter Reed Army Hospital; and Paul Wender, Ph.D., of Stanford University.
In addition to its technical resources, iDDi is developing a novel operational model aimed at making practical and affordable medicines available to those in need. To this end, Mohsen Marefat of The Althing Group has been retained to head the development and management of business operations for the Institute.
To date, iDDi has been funded by donations from angel benefactors. The Institute plans to launch an aggressive fundraising campaign to attract foundation support.
About iDDi
iDDi is a non-profit institute that will accelerate and streamline drug discovery by harnessing the power of technology and the expertise of select scientists, worldwide, to identify and bring to market effective and practical therapies for diseases afflicting millions. For more information, please visit www.i-ddi.org.
Thursday, 13 September 2007
XDR-TB in Western Pacific Region
A top World Health Organization (WHO) official urged Asia-Pacific countries on Wednesday to step up their fight against growing outbreaks of multidrug-resistant tuberculosis.
Shigeru Omi, regional director for the Western Pacific, also called for immediate action to prevent the development of extensively drug resistant-TB or XDR-TB in the region.
"There is an urgent need to scale up the management of multidrug resistant-TB, which has emerged across the region, including the Pacific," said Omi.
The region has about a third of the global multidrug resistant-TB burden, mostly in China and the Philippines, and to some extent in Mongolia, South Korea and Vietnam, according to the WHO.
Tuberculosis of all kinds continues to be a major public health problem in the Western Pacific with an estimated 1.9 million new cases in 2005.
"The potential magnitude of the threat of multidrug-resistant TB in the region requires countries to urgently develop a response and thus prevent the development of extensively drug resistant-TB or XDR-TB," Omi said.
Omi also drew attention to "increasing concern" about HIV-related TB, saying that in the region TB is the main opportunistic infection that kills people living with HIV/AIDS.
He called for comprehensive infection control strategies to prevent the spread of TB among HIV sufferers.
The meeting heard that access to HIV treatment continues to expand in the region but significant obstacles to universal access must still be overcome.
In the Western Pacific 1.3 million people were living with HIV at the end of 2006 and almost 80,000 died of HIV/AIDS that year.
"Despite some success in scaling up prevention interventions, the epidemic continues to grow, with an estimated 167,000 new HIV infections occurring in the region in 2006," a statement said.
http://afp.google.com/article/ALeqM5jggbQbTMcbUiGz_Q_e8z6D1_oLzA
Shigeru Omi, regional director for the Western Pacific, also called for immediate action to prevent the development of extensively drug resistant-TB or XDR-TB in the region.
"There is an urgent need to scale up the management of multidrug resistant-TB, which has emerged across the region, including the Pacific," said Omi.
The region has about a third of the global multidrug resistant-TB burden, mostly in China and the Philippines, and to some extent in Mongolia, South Korea and Vietnam, according to the WHO.
Tuberculosis of all kinds continues to be a major public health problem in the Western Pacific with an estimated 1.9 million new cases in 2005.
"The potential magnitude of the threat of multidrug-resistant TB in the region requires countries to urgently develop a response and thus prevent the development of extensively drug resistant-TB or XDR-TB," Omi said.
Omi also drew attention to "increasing concern" about HIV-related TB, saying that in the region TB is the main opportunistic infection that kills people living with HIV/AIDS.
He called for comprehensive infection control strategies to prevent the spread of TB among HIV sufferers.
The meeting heard that access to HIV treatment continues to expand in the region but significant obstacles to universal access must still be overcome.
In the Western Pacific 1.3 million people were living with HIV at the end of 2006 and almost 80,000 died of HIV/AIDS that year.
"Despite some success in scaling up prevention interventions, the epidemic continues to grow, with an estimated 167,000 new HIV infections occurring in the region in 2006," a statement said.
http://afp.google.com/article/ALeqM5jggbQbTMcbUiGz_Q_e8z6D1_oLzA
From Northern Canada
Members of a major health project in Nunavut are holding a ceremony on Tuesday to remember Inuit who lost their lives to tuberculosis in the 1950s and '60s.
The Nunavut Inuit Health Survey —— known as Qanuippitali?, which is Inuktitut for, "How about us, how are we?" —— is hosting a commemoration ceremony in Apex, near Iqaluit, at 2 p.m. ET. The event is expected to include a drum dance, speeches by elders, and an unveiling of a plaque.
During the project, 40 doctors, nurses, lab technicians and interpreters, along with 40 coast guard personnel, have been travelling to 19 coastal communities around the territory in August and September aboard a "floating health lab" on the icebreaker Amundsen.
They bring Inuit on board the Amundsen for three-hour medical appointments. Randomly selected participants are asked fill out questionnaires and undergo medical tests for diseases such as diabetes and stroke.
Survey lead Prof. Dr. Grace Egeland of McGill University said the project raised memories of the C.D. Howe medical ship in the 1950s, which gathered about 1,600 Inuit tuberculosis patients and transported them to sanatoriums in southern Canada. Many of those patients never returned.
"As we were planning this survey using the ship, the memories of C.D. Howe have come back to people in communities," Egeland told CBC News on Monday. "There's been no closure, no healing, no group ceremony where we can collectively come together to recognize the loss and the tragedy and the suffering of families."
Egeland said she hopes Tuesday's event will emphasize a positive change in working relationships with Inuit.
http://www.cbc.ca/health/story/2007/09/11/nu_tb.html
The Nunavut Inuit Health Survey —— known as Qanuippitali?, which is Inuktitut for, "How about us, how are we?" —— is hosting a commemoration ceremony in Apex, near Iqaluit, at 2 p.m. ET. The event is expected to include a drum dance, speeches by elders, and an unveiling of a plaque.
During the project, 40 doctors, nurses, lab technicians and interpreters, along with 40 coast guard personnel, have been travelling to 19 coastal communities around the territory in August and September aboard a "floating health lab" on the icebreaker Amundsen.
They bring Inuit on board the Amundsen for three-hour medical appointments. Randomly selected participants are asked fill out questionnaires and undergo medical tests for diseases such as diabetes and stroke.
Survey lead Prof. Dr. Grace Egeland of McGill University said the project raised memories of the C.D. Howe medical ship in the 1950s, which gathered about 1,600 Inuit tuberculosis patients and transported them to sanatoriums in southern Canada. Many of those patients never returned.
"As we were planning this survey using the ship, the memories of C.D. Howe have come back to people in communities," Egeland told CBC News on Monday. "There's been no closure, no healing, no group ceremony where we can collectively come together to recognize the loss and the tragedy and the suffering of families."
Egeland said she hopes Tuesday's event will emphasize a positive change in working relationships with Inuit.
http://www.cbc.ca/health/story/2007/09/11/nu_tb.html
More on XDR-TB and Andrew Speaker
At the request of Committee on Homeland Security Chairman Bennie G. Thompson (D-MS), the Majority Staff of the Committee on Homeland Security published a comprehensive report which analyzes the federal government's trouble with handling an XDR-TB case and the government's ability to manage incidents like it.
The report concludes that many of the problems associated with the conducting of the case have still not been resolved.
Specifically, the report looks into the interactions between the Department of Homeland Security and the Centers for Disease Control and Prevention (CDC) regarding public health security issues, while identifying weaknesses in homeland security processes designed to prevent "persons of interest" from entering the United States and making recommendations for improvements to the federal handling of national security on the nation's home soil.
"This was a real world incident, and there was a breakdown at the intersection of homeland security and public health. The government has numerous plans and policies in place to secure our communities, but they just didn't follow the playbook. This certainly raises questions about our homeland security if the government had this much trouble countering TB, let alone countering terrorism," said Thompson.
The case in question centers on a 31-year-old American Lawyer named Andrew Speaker.
Speaker learned he had tuberculosis, or TB, in January of this year. In May, his doctors realized that he had XDR-TB, which is a fiercely drug-resistant strain of the illness. He was permitted to board a commercial flight to Paris on May the 12th , and returned from Europe 12 days later on a flight into Canada from Prague in the Czech Republic.
Speaker said that he had begun feeling better by the time of his flight and never realized he had something in his body that could infect or harm anyone else.
His doctors told Speaker not to travel, but Speaker maintains that while the Centers for Disease Control and Prevention as well as other health organizations advised him against travel, they did nothing to stop him and did not describe to him in detail what he was carrying.
XDR-TB is "extensively drug-resistant tuberculosis". One in three people in the world is infected with dormant TB germs (bacteria). The bacteria have to become active before people become ill with TB.
The bacteria become active as a result of anything that can reduce a person's immunity, such as HIV, aging into advanced years, or certain pre-existing medical conditions. TB can typically be treated with a course of four standard or "first-line" anti-TB drugs However, multidrug-resistant tuberculosis (MDR-TB) takes longer to treat and demands the use of second-line drugs, which are more expensive and have more side-effects than first-line drugs. If drugs get misused or misapplied in treating TB, then XDR-TB can develop.
Due to the fact that XDR-TB is resistant to first- and second-line drugs, treatment options are severely limited, and a person with the illness has to be strictly managed to prevent the spread of the potentially fatal illness.
The report concludes that many of the problems associated with the conducting of the case have still not been resolved.
Specifically, the report looks into the interactions between the Department of Homeland Security and the Centers for Disease Control and Prevention (CDC) regarding public health security issues, while identifying weaknesses in homeland security processes designed to prevent "persons of interest" from entering the United States and making recommendations for improvements to the federal handling of national security on the nation's home soil.
"This was a real world incident, and there was a breakdown at the intersection of homeland security and public health. The government has numerous plans and policies in place to secure our communities, but they just didn't follow the playbook. This certainly raises questions about our homeland security if the government had this much trouble countering TB, let alone countering terrorism," said Thompson.
The case in question centers on a 31-year-old American Lawyer named Andrew Speaker.
Speaker learned he had tuberculosis, or TB, in January of this year. In May, his doctors realized that he had XDR-TB, which is a fiercely drug-resistant strain of the illness. He was permitted to board a commercial flight to Paris on May the 12th , and returned from Europe 12 days later on a flight into Canada from Prague in the Czech Republic.
Speaker said that he had begun feeling better by the time of his flight and never realized he had something in his body that could infect or harm anyone else.
His doctors told Speaker not to travel, but Speaker maintains that while the Centers for Disease Control and Prevention as well as other health organizations advised him against travel, they did nothing to stop him and did not describe to him in detail what he was carrying.
XDR-TB is "extensively drug-resistant tuberculosis". One in three people in the world is infected with dormant TB germs (bacteria). The bacteria have to become active before people become ill with TB.
The bacteria become active as a result of anything that can reduce a person's immunity, such as HIV, aging into advanced years, or certain pre-existing medical conditions. TB can typically be treated with a course of four standard or "first-line" anti-TB drugs However, multidrug-resistant tuberculosis (MDR-TB) takes longer to treat and demands the use of second-line drugs, which are more expensive and have more side-effects than first-line drugs. If drugs get misused or misapplied in treating TB, then XDR-TB can develop.
Due to the fact that XDR-TB is resistant to first- and second-line drugs, treatment options are severely limited, and a person with the illness has to be strictly managed to prevent the spread of the potentially fatal illness.
Tuesday, 11 September 2007
Tuberculosis in Africa -- incomplete data
The World Health Organisation said lack of regional data for Tuberculosis (TB) prevalence in Africa is hampering the monitoring and evaluation of TB control programmes there and was hampering health officials in efforts to estimate the disease prevalence, unlike HIV, which has regional records to facilitate planning to control the spread of the pandemic.
Some 590,000 Africans die from Tuberculosis annually, this is 35% of the world total. Africans living with TB are estimated to be around 4 million.
Despite the significant progress by member states in the implementing of the Direct Observed Therapy Short (DOTS) course, TB remained the most important communicable disease in the Region. Other challenges faced by the region to control TB were low or non-participation of the private sector, limited laboratory facilities for diagnosis, human resource capacity, slow country TB/HIV implementation and the expansion of community and civil society Organizations involvement.
Outlining some strategic ways to address the challenges, WHO African Regional Office suggested pragmatic actions to accelerate population DOTS coverage to increase case detection, reduce patient default to improve treatment success rates and strengthening health systems for TB laboratory networks as well as mobilising additional resources for TB. WHO Africa Regional Office would ensure the reduction of the gap created between policy and implementation, advocate for correct approach to programme implementation, undertake special studies on TB prevalence and DOTS implementation and make available simple treatment guidelines and charts. These strategies would help to achieve the global target of stopping TB by at least 70 per cent case detection rate and 85 per cent treatment success rate among new cases by 2015.
http://www.afriquenligne.fr/news/daily_news/who_says_africa_region_lacks_data_on_tb_prevalence_200709108303/
Some 590,000 Africans die from Tuberculosis annually, this is 35% of the world total. Africans living with TB are estimated to be around 4 million.
Despite the significant progress by member states in the implementing of the Direct Observed Therapy Short (DOTS) course, TB remained the most important communicable disease in the Region. Other challenges faced by the region to control TB were low or non-participation of the private sector, limited laboratory facilities for diagnosis, human resource capacity, slow country TB/HIV implementation and the expansion of community and civil society Organizations involvement.
Outlining some strategic ways to address the challenges, WHO African Regional Office suggested pragmatic actions to accelerate population DOTS coverage to increase case detection, reduce patient default to improve treatment success rates and strengthening health systems for TB laboratory networks as well as mobilising additional resources for TB. WHO Africa Regional Office would ensure the reduction of the gap created between policy and implementation, advocate for correct approach to programme implementation, undertake special studies on TB prevalence and DOTS implementation and make available simple treatment guidelines and charts. These strategies would help to achieve the global target of stopping TB by at least 70 per cent case detection rate and 85 per cent treatment success rate among new cases by 2015.
http://www.afriquenligne.fr/news/daily_news/who_says_africa_region_lacks_data_on_tb_prevalence_200709108303/
Tuberculosis in Central Asia Prisons
In the majority of Central Asia's prisons and colonies, inmate access to even basic medical care is severely limited. Rights activists and former convicts say sick prisoners often get only one-half or even one-quarter of a pain-relief tablet, regardless of what illness they have. Prison facilities are considered the epidemiological pump behind the high rate of infectious diseases there.
The rates of HIV/AIDS and tuberculosis (TB) are high among inmates. The Brussels-based International Crisis Group reported last year that cases of TB among prisoners has more than doubled in Kazakhstan, tripled in Uzbekistan, and increased fivefold in Tajikistan since 1990.
In Kyrgyzstan, the rates of TB among prison inmates are said to be 40 times higher than in the general population and mortality rates are some 60 times higher, the ICG reported.
In response to this alarming situation, Kyrgyz authorities seem to be taking steps to address the problem. Observers have said that TB -- particularly its drug-resistant strains -- is rampant, two of the three prisons for men that have TB hospitals in Kyrgyzstan. (The women's and juveniles' colonies also house TB treatment centers.)
Kyrgyz authorities have demonstrated commitment and maturity in dealing with contagious diseases in the penal system. "Like all other prisons in this region, the situation [in Kyrgyz prisons] and the conditions of sick [convicts] are very bad, however, Kyrgyzstan does much more compared to other countries of the region in order to reduce the threat of the penitentiary system as a source of tuberculosis and HIV/AIDS."
Kyrgyzstan was the first country in Central Asia to receive the Global Fund's financial aid to start treatment of people with multidrug-resistant tuberculosis.
Central Asian countries are situated on a transit route of narcotics from Afghanistan to Russia and on to Europe. All of them, including Kyrgyzstan, have seen a sharp increase in the number of drug addicts -- particularly heroin users -- in recent years. The trend has led to the rise of HIV/AIDS among the general population, as well as in prisons.
"Yesterday, when we visited it, there were 52 people in a place suited for only 30 people. Their conditions were hard. There was neither fresh air, nor natural light [in the cells]. Food was provided for 30 people; the other 22 people did not receive any."
In general, convicts lack basic medical care as well. Specialized services, like oncological, gynecological, mental, and dental services are virtually unavailable in most prisons in the region. Nutritious food -- a key in treating TB -- is also in very short supply.
Furthermore, prisoners who receive treatment for TB in prisons and who require further therapy do not receive follow-up care. Thus, they are likely to spread TB among the general population after their release from prison.
http://www.rferl.org/featuresarticle/2007/09/5A8A687A_1826_42A9_82E6_3E8FC809F5FD.html
The rates of HIV/AIDS and tuberculosis (TB) are high among inmates. The Brussels-based International Crisis Group reported last year that cases of TB among prisoners has more than doubled in Kazakhstan, tripled in Uzbekistan, and increased fivefold in Tajikistan since 1990.
In Kyrgyzstan, the rates of TB among prison inmates are said to be 40 times higher than in the general population and mortality rates are some 60 times higher, the ICG reported.
In response to this alarming situation, Kyrgyz authorities seem to be taking steps to address the problem. Observers have said that TB -- particularly its drug-resistant strains -- is rampant, two of the three prisons for men that have TB hospitals in Kyrgyzstan. (The women's and juveniles' colonies also house TB treatment centers.)
Kyrgyz authorities have demonstrated commitment and maturity in dealing with contagious diseases in the penal system. "Like all other prisons in this region, the situation [in Kyrgyz prisons] and the conditions of sick [convicts] are very bad, however, Kyrgyzstan does much more compared to other countries of the region in order to reduce the threat of the penitentiary system as a source of tuberculosis and HIV/AIDS."
Kyrgyzstan was the first country in Central Asia to receive the Global Fund's financial aid to start treatment of people with multidrug-resistant tuberculosis.
Central Asian countries are situated on a transit route of narcotics from Afghanistan to Russia and on to Europe. All of them, including Kyrgyzstan, have seen a sharp increase in the number of drug addicts -- particularly heroin users -- in recent years. The trend has led to the rise of HIV/AIDS among the general population, as well as in prisons.
"Yesterday, when we visited it, there were 52 people in a place suited for only 30 people. Their conditions were hard. There was neither fresh air, nor natural light [in the cells]. Food was provided for 30 people; the other 22 people did not receive any."
In general, convicts lack basic medical care as well. Specialized services, like oncological, gynecological, mental, and dental services are virtually unavailable in most prisons in the region. Nutritious food -- a key in treating TB -- is also in very short supply.
Furthermore, prisoners who receive treatment for TB in prisons and who require further therapy do not receive follow-up care. Thus, they are likely to spread TB among the general population after their release from prison.
http://www.rferl.org/featuresarticle/2007/09/5A8A687A_1826_42A9_82E6_3E8FC809F5FD.html
Monday, 10 September 2007
Memories of Sanatorium life in Wales
The exhibition has been organised by a former patient at the Adelina Patti Hospital in the Swansea Valley, better known as Craig-y-nos Castle, it housed TB patients from 1922-59.
Craig-y-nos Castle was the estate of the world-renowned opera singer Adelina Patti until her death in 1919.
Two years later, it was bought by an organisation founded to combat TB in Wales and was reconstructed as a sanatorium before admitting its first patients in August 1922.
The exhibition is part of an oral history project supported by the Heritage Lottery Fund and the Sleeping Giant Foundation charity.
"It will be the first ever collective account by patients and staff of life inside a tuberculosis sanatorium and is therefore a unique heritage project."
"The time period, from the 1920s to the 1950s, is also crucial because of the tremendous activity by medical professionals and other groups to understand the nature of tuberculosis.
"The real treatment breakthrough came in 1947 when the first effective medicine, an antibiotic called streptomycin, became available in Britain. The children of Craig-y-nos were among the first to receive this new 'wonder' drug. "
http://news.bbc.co.uk/1/hi/wales/south_west/6984547.stm
Craig-y-nos Castle was the estate of the world-renowned opera singer Adelina Patti until her death in 1919.
Two years later, it was bought by an organisation founded to combat TB in Wales and was reconstructed as a sanatorium before admitting its first patients in August 1922.
The exhibition is part of an oral history project supported by the Heritage Lottery Fund and the Sleeping Giant Foundation charity.
"It will be the first ever collective account by patients and staff of life inside a tuberculosis sanatorium and is therefore a unique heritage project."
"The time period, from the 1920s to the 1950s, is also crucial because of the tremendous activity by medical professionals and other groups to understand the nature of tuberculosis.
"The real treatment breakthrough came in 1947 when the first effective medicine, an antibiotic called streptomycin, became available in Britain. The children of Craig-y-nos were among the first to receive this new 'wonder' drug. "
http://news.bbc.co.uk/1/hi/wales/south_west/6984547.stm
Failure of follow-up in Taiwan -- Is it any better in America?
A doctor with the Department of Health's Chest Hospital in Taipei warned on Wednesday that the country's efforts to battle tuberculosis have a weak link because 90 percent of those in close contact with TB patients are not thoroughly tested. He said new regulations on TB control that took effect in June require anyone who has been in contact with an infectious TB patient for eight hours in a single day to be tested for infection. Between August 2005 and July, there were 1,069 people who required such testing. However, after having an initial chest X-ray taken, 969 never returned for a second check-up. Only 89 had a second chest X-ray taken within the next year, while just 11 returned for a third test.
The bacteria that causes TB can remain dormant for many years, and that those who are infected have a 10 percent to 20 percent chance of developing the disease, while half of these will become symptomatic within five years.
TB is the most prevalent communicable disease in Taiwan. Approximately 15,000 persons are infected every year.
Statistics show that there were 24,161 people with TB in 2004, including 16,784 new cases, an incidence rate of 74.11 per 100,000 people. About 92.3 percent of the cases were pulmonary TB. That year 957 people died of the disease.
http://www.taipeitimes.com/News/taiwan/archives/2007/09/07/2003377587
The bacteria that causes TB can remain dormant for many years, and that those who are infected have a 10 percent to 20 percent chance of developing the disease, while half of these will become symptomatic within five years.
TB is the most prevalent communicable disease in Taiwan. Approximately 15,000 persons are infected every year.
Statistics show that there were 24,161 people with TB in 2004, including 16,784 new cases, an incidence rate of 74.11 per 100,000 people. About 92.3 percent of the cases were pulmonary TB. That year 957 people died of the disease.
http://www.taipeitimes.com/News/taiwan/archives/2007/09/07/2003377587
Nepalese student dies of TB in Colorado
Local health department officials are urging Colorado State University-Pueblo students and staff who had close contact with a student who died of tuberculosis in June to be tested again for the communicable disease. The follow-up TB test is only for those individuals who have been identified as having close contact with the victim and who tested negative on the first test administered in late June.
On June 8, CSU-Pueblo international student Kalpana Dangol died of tuberculosis at Memorial Hospital in Colorado Springs. Dangol, a native of Nepal, attended CSU-Pueblo for three semesters, including spring 2007. She never lived on campus and at the time of her death, she was living with her sister in Colorado Springs.
In late June, the Pueblo and El Paso county health departments hosted free TB clinics for the 160 individuals who were identified as having close contact with Dangol. The first clinic was well-attended but those needing the follow-up test have not responded as health officials would like them to. Enough time has passed that if an individual is carrying TB, a test now will show a positive result. "If it shows positive, that doesn't necessarily mean that you have active TB but that you may have been exposed to someone with active TB, a positive result does not necessarily mean a person is contagious, but would indicate the need for further testing and precautionary treatment."
"These services are all free of charge and it's so important, not only for your health but also for your peace of mind."
http://www.chieftain.com/metro/1189151658/6
On June 8, CSU-Pueblo international student Kalpana Dangol died of tuberculosis at Memorial Hospital in Colorado Springs. Dangol, a native of Nepal, attended CSU-Pueblo for three semesters, including spring 2007. She never lived on campus and at the time of her death, she was living with her sister in Colorado Springs.
In late June, the Pueblo and El Paso county health departments hosted free TB clinics for the 160 individuals who were identified as having close contact with Dangol. The first clinic was well-attended but those needing the follow-up test have not responded as health officials would like them to. Enough time has passed that if an individual is carrying TB, a test now will show a positive result. "If it shows positive, that doesn't necessarily mean that you have active TB but that you may have been exposed to someone with active TB, a positive result does not necessarily mean a person is contagious, but would indicate the need for further testing and precautionary treatment."
"These services are all free of charge and it's so important, not only for your health but also for your peace of mind."
http://www.chieftain.com/metro/1189151658/6
Tuberculosis control in the Philippines
The Philippine Government is doubling its tuberculosis control budget to P280 million next year to combat a resurgent disease which is said to infect six in ten Filipinos and claims one life every 20 minutes in the country. 100-percent hike in funds of the Department of Health TB Control Program this year which is P139 million has been included in the proposed national budget. This would allow the government to procure more anti-TB drugs, which are mainly administered to patients through the proven Directly-Observed Treatment Short Course (DOTS).
The Provincial Health Office here has taken a more vigorous approach to combat tuberculosis, like early detection through sputum examination, laboratory and x-ray services.
The Multi-Drug-Resistant (MDR) cases are also covered by the program (DOTS). These are TB cases that despite the medication, patients when subjected to sputum examination were still found to be positive of the disease.
More attention would be given to this category as these were described to be expensive to treat or cure, very contagious and noted to be responsible for spreading TB resistant bacilli. TB cases of this nature qualify for referral to Makati Tropical Disease Foundation Clinic, so patients could be subjected to thorough medication, but the process entails enormous amount of money, a longer period of treatment as Out-Patient.
http://www.pia.gov.ph/?m=12&fi=p070906.htm&no=44
The Provincial Health Office here has taken a more vigorous approach to combat tuberculosis, like early detection through sputum examination, laboratory and x-ray services.
The Multi-Drug-Resistant (MDR) cases are also covered by the program (DOTS). These are TB cases that despite the medication, patients when subjected to sputum examination were still found to be positive of the disease.
More attention would be given to this category as these were described to be expensive to treat or cure, very contagious and noted to be responsible for spreading TB resistant bacilli. TB cases of this nature qualify for referral to Makati Tropical Disease Foundation Clinic, so patients could be subjected to thorough medication, but the process entails enormous amount of money, a longer period of treatment as Out-Patient.
http://www.pia.gov.ph/?m=12&fi=p070906.htm&no=44
Tuberculosis in Zaire province of Northern Angola
Health authorities in the northern Zaire Province recorded at least 766 cases of tuberculosis in the first semester of this year, including three deaths caused by that disease.
According to an official, in comparison to the second semester of last year there was a decrease of 50 TB cases, with the most affected age group being those between 24 to 45 years old. As factors that contribute to the high number of TB cases in the province, he pointed out the poor social conditions of many families and the excessive use of alcoholic drinks.
http://allafrica.com/stories/200709060818.html
According to an official, in comparison to the second semester of last year there was a decrease of 50 TB cases, with the most affected age group being those between 24 to 45 years old. As factors that contribute to the high number of TB cases in the province, he pointed out the poor social conditions of many families and the excessive use of alcoholic drinks.
http://allafrica.com/stories/200709060818.html
Control of neonatal tuberculosis in Africa
The call to action in Prevention of Mother to Child Transmission (PMTCT) aims to reduce the risk of mother to child transmission of HIV through integrated HIV/Aids education, routine counselling and testing as well as administration of a prophylaxis single dose Nevirapine therapy to mother and infant.
It goes without saying then, that the need to protect infants or the unborn from the possibility of contracting Tuberculosis, including the Multi-Drug Resistant (MDR) and Extremely Drug Resistant (XDR) TB, which is closely linked to the HIV epidemic, becomes of paramount importance.
During the last decade, there has been an increase of TB infections as an opportunistic infection in people with HIV because of their weakened immune systems. This is causing concern in the light of MDR and XDR-TB surfacing because interventions such as the prevention of mother to child transmission of HIV may be challenged where the mother is living with HIV and found with Tuberculosis.
Communications Officer of National TB Control Programme, Henry Chimbali, told Health Check that most healthy people do not get TB unless they are in very close contact with people infected with Tuberculosis as it is spread through droplets in the air.
"The infection of XDR-TB is transmitted the same as the standard TB and could be prevented the same way ordinary Tuberculosis is prevented," Chimbali said.
The international medical humanitarian organisation, Medicines Sans Frontieres (MSF) is quoted by Health Check calling for approaches and new tools to treat multi-drug resistant (MDR) Tuberculosis in Southern Africa.
"MDR, and now XDR-TB, are the tip of an iceberg of failing strategies to control TB," said Dr.. Eric Goemaere of MSF "We desperately need new tools and new approaches and we need them now - we cannot just sit and wait. Despite all the international fanfare created by XDR, efforts to treat drug resistant TB in high HIV prevalence settings are moving at a snail's pace and investments to develop new drugs and diagnostics to improve management of all forms of TB are terribly inadequate. This situation is unacceptable."
Chimbali told Health Check, however, that any development of TB could be averted if regular TB is treated effectively and if Malawi succeeded in controlling the XDR-TB transmission, then the risk of infection would not be there.
Country Director for UNC Project at Kamuzu Central Hospital, Dr.. Francis Martinson, says there is need for a prophylaxis regimen to protect mother/infant pairs from tuberculosis just as there is a Nevirapine dose to facilitate the prevention of mother to child transmission of HIV.
In this regard, University of Northern Carolina (UNC) Project has embarked on a randomized, placebo-controlled trial to determine the efficacy of Isoniazid (INH), a component drug in the combination of TB treatment in preventing Tuberculosis disease and latent TB infection among South African infants with peri-natal exposure to HIV.
Dr. Martinson told Health Check that the trial would have an initial sample size of 1,300 study participants consisting of 500 infected and 800 uninfected exposed study participants.
"The objective of the trial aims to determine whether INH prophylaxis increases TB disease survival for HIV infected participants; to determine whether INH prophylaxis increases TB infection-free survival for peri-natal-exposed HIV uninfected study participants," said Dr.. Martinson.
"Among both peri-natal-exposed HIV infected and HIV uninfected study participants we are also trying to assess the toxicity and safety of INH prophylaxis."
The fact that once one is HIV positive and having Tuberculosis, one is automatically placed on antiretroviral therapy, puts the mother/infant pair at risk of not accessing medical care if they infect one another and do not get diagnosed in time.
http://allafrica.com/stories/200709040470.html
It goes without saying then, that the need to protect infants or the unborn from the possibility of contracting Tuberculosis, including the Multi-Drug Resistant (MDR) and Extremely Drug Resistant (XDR) TB, which is closely linked to the HIV epidemic, becomes of paramount importance.
During the last decade, there has been an increase of TB infections as an opportunistic infection in people with HIV because of their weakened immune systems. This is causing concern in the light of MDR and XDR-TB surfacing because interventions such as the prevention of mother to child transmission of HIV may be challenged where the mother is living with HIV and found with Tuberculosis.
Communications Officer of National TB Control Programme, Henry Chimbali, told Health Check that most healthy people do not get TB unless they are in very close contact with people infected with Tuberculosis as it is spread through droplets in the air.
"The infection of XDR-TB is transmitted the same as the standard TB and could be prevented the same way ordinary Tuberculosis is prevented," Chimbali said.
The international medical humanitarian organisation, Medicines Sans Frontieres (MSF) is quoted by Health Check calling for approaches and new tools to treat multi-drug resistant (MDR) Tuberculosis in Southern Africa.
"MDR, and now XDR-TB, are the tip of an iceberg of failing strategies to control TB," said Dr.. Eric Goemaere of MSF "We desperately need new tools and new approaches and we need them now - we cannot just sit and wait. Despite all the international fanfare created by XDR, efforts to treat drug resistant TB in high HIV prevalence settings are moving at a snail's pace and investments to develop new drugs and diagnostics to improve management of all forms of TB are terribly inadequate. This situation is unacceptable."
Chimbali told Health Check, however, that any development of TB could be averted if regular TB is treated effectively and if Malawi succeeded in controlling the XDR-TB transmission, then the risk of infection would not be there.
Country Director for UNC Project at Kamuzu Central Hospital, Dr.. Francis Martinson, says there is need for a prophylaxis regimen to protect mother/infant pairs from tuberculosis just as there is a Nevirapine dose to facilitate the prevention of mother to child transmission of HIV.
In this regard, University of Northern Carolina (UNC) Project has embarked on a randomized, placebo-controlled trial to determine the efficacy of Isoniazid (INH), a component drug in the combination of TB treatment in preventing Tuberculosis disease and latent TB infection among South African infants with peri-natal exposure to HIV.
Dr. Martinson told Health Check that the trial would have an initial sample size of 1,300 study participants consisting of 500 infected and 800 uninfected exposed study participants.
"The objective of the trial aims to determine whether INH prophylaxis increases TB disease survival for HIV infected participants; to determine whether INH prophylaxis increases TB infection-free survival for peri-natal-exposed HIV uninfected study participants," said Dr.. Martinson.
"Among both peri-natal-exposed HIV infected and HIV uninfected study participants we are also trying to assess the toxicity and safety of INH prophylaxis."
The fact that once one is HIV positive and having Tuberculosis, one is automatically placed on antiretroviral therapy, puts the mother/infant pair at risk of not accessing medical care if they infect one another and do not get diagnosed in time.
http://allafrica.com/stories/200709040470.html
Tuberculosis infection rates among international adoptees
Tuberculosis infection rates among international adoptees to the United States has risen dramatically over the past 20 years, according to new findings which add weight to a call for Canada to screen all incoming adoptees for the disease.
The American study followed up on 869 foreign-born children adopted into U.S. families from 1986 through 2001. Twelve per cent of the children were infected with tuberculosis and the rate of TB infections among the adoptees rose seven per cent with each passing year through the period studied.
"These kids are getting infected very, very early in life," said lead author Dr. Anna Mandalakas, who runs the adoption health service at Rainbow Babies and Children's Hospital in Cleveland, Ohio. "So during this first two years of life if they're in an orphanage, a huge number of these children are getting infected."
The authors of the study, which was published Tuesday in the journal Pediatrics, say the findings support the current call from the American Academy of Pediatrics that all international adoptees undergo a skin test for tuberculosis immediately after adoption.
Two Canadian tuberculosis experts recently urged that TB screening policy for international adoptees be instituted in Canada, suggesting in a commentary in the Canadian Medical Association Journal that provinces and territories should follow up with adoptive parents to ensure these children get timely and thorough testing.
TB rates among the children in the American study ranged from nearly 15 per cent in adoptees from Eastern Europe, 14 per cent from Russia and 13 per cent from Korea to between 12.5 per cent and 11 per cent in India, China and South America, 8.3 per cent in Central America and the Caribbean and 2.8 per cent in Southeast Asia.
Canadians routinely adopt children from these same regions or countries, some of which have among the highest rates of tuberculosis globally. According to Citizenship and Immigration Canada, an average of 2,000 children a year are adopted into Canadian families from abroad.
The medical examination required of immigrants to Canada isn't geared towards detecting latent tuberculosis infection or TB disease in children under 11 years of age, Dr. Richard Long and co-author Jody Boffa of the tuberculosis program evaluation and research unit at the University of Alberta wrote in the Canadian Medical Association Journal earlier this summer.
But given the risk faced by international adoptees, this special group ought to be screened, Long and Boffa suggested. Their commentary noted that four in 10 foreign-born children under the age of five found to be infected with tuberculosis in Alberta between 2004 and 2006 were international adoptees.
Long said children infected with latent or even active TB don't pose a risk to others, because children under nine or 10 years of age rarely transmit disease. But the infection is a real threat to their own health, he said in an interview.
Infection with Mycobacterium tuberculosis, the bug that causes TB, doesn't always lead to active disease. In many people the bacteria remains latent. Infected adults have about a five to 10 per cent chance of developing active tuberculosis sometime in their lifetime.
With young children, however, the risk that infection will lead to disease is much higher. Infants under a year have a roughly 50 per cent chance of developing disease and children aged one to two have a 20 per cent chance. And if active TB develops, it can progress beyond the lungs, the typical site of disease.
"Little children not only have a higher risk of getting disease from infection itself, they're at higher risk of getting severe forms of disease - and by severe forms I mean central nervous system or disseminated TB," said Long, who also serves as Alberta's medical officer of health for tuberculosis.
A TB expert at Toronto's University Health Network agreed.
"They're a relatively small population, but they're a really high risk population," said Dr. Michael Gardam, who is head of infection control for that network of three central Toronto hospitals. Gardam was not involved in either the study or the commentary.
"Because these kids are not coming from healthy, happy homes. They're coming from environments where they're very likely to have been exposed to tuberculosis. And I think it makes perfect sense to be screening them."
Both Mandalakas' study and Long's commentary recommend the screening begin swiftly after an international adoptee arrives in his or her new home.
And both recommended that the initial skin test be followed up three to six months later with another. That's because a test performed immediately after arrival might not detect an infection that occurred shortly before a child left an overseas orphanage.
Children who test positive should be put on a nine month course of antibiotics, Mandalakas said. She also suggested orphanages involved in international adoptions should test for tuberculosis among employees.
http://canadianpress.google.com/article/ALeqM5g_3TL6bspoGhwMS_sb1_nbv6KAeQ
The American study followed up on 869 foreign-born children adopted into U.S. families from 1986 through 2001. Twelve per cent of the children were infected with tuberculosis and the rate of TB infections among the adoptees rose seven per cent with each passing year through the period studied.
"These kids are getting infected very, very early in life," said lead author Dr. Anna Mandalakas, who runs the adoption health service at Rainbow Babies and Children's Hospital in Cleveland, Ohio. "So during this first two years of life if they're in an orphanage, a huge number of these children are getting infected."
The authors of the study, which was published Tuesday in the journal Pediatrics, say the findings support the current call from the American Academy of Pediatrics that all international adoptees undergo a skin test for tuberculosis immediately after adoption.
Two Canadian tuberculosis experts recently urged that TB screening policy for international adoptees be instituted in Canada, suggesting in a commentary in the Canadian Medical Association Journal that provinces and territories should follow up with adoptive parents to ensure these children get timely and thorough testing.
TB rates among the children in the American study ranged from nearly 15 per cent in adoptees from Eastern Europe, 14 per cent from Russia and 13 per cent from Korea to between 12.5 per cent and 11 per cent in India, China and South America, 8.3 per cent in Central America and the Caribbean and 2.8 per cent in Southeast Asia.
Canadians routinely adopt children from these same regions or countries, some of which have among the highest rates of tuberculosis globally. According to Citizenship and Immigration Canada, an average of 2,000 children a year are adopted into Canadian families from abroad.
The medical examination required of immigrants to Canada isn't geared towards detecting latent tuberculosis infection or TB disease in children under 11 years of age, Dr. Richard Long and co-author Jody Boffa of the tuberculosis program evaluation and research unit at the University of Alberta wrote in the Canadian Medical Association Journal earlier this summer.
But given the risk faced by international adoptees, this special group ought to be screened, Long and Boffa suggested. Their commentary noted that four in 10 foreign-born children under the age of five found to be infected with tuberculosis in Alberta between 2004 and 2006 were international adoptees.
Long said children infected with latent or even active TB don't pose a risk to others, because children under nine or 10 years of age rarely transmit disease. But the infection is a real threat to their own health, he said in an interview.
Infection with Mycobacterium tuberculosis, the bug that causes TB, doesn't always lead to active disease. In many people the bacteria remains latent. Infected adults have about a five to 10 per cent chance of developing active tuberculosis sometime in their lifetime.
With young children, however, the risk that infection will lead to disease is much higher. Infants under a year have a roughly 50 per cent chance of developing disease and children aged one to two have a 20 per cent chance. And if active TB develops, it can progress beyond the lungs, the typical site of disease.
"Little children not only have a higher risk of getting disease from infection itself, they're at higher risk of getting severe forms of disease - and by severe forms I mean central nervous system or disseminated TB," said Long, who also serves as Alberta's medical officer of health for tuberculosis.
A TB expert at Toronto's University Health Network agreed.
"They're a relatively small population, but they're a really high risk population," said Dr. Michael Gardam, who is head of infection control for that network of three central Toronto hospitals. Gardam was not involved in either the study or the commentary.
"Because these kids are not coming from healthy, happy homes. They're coming from environments where they're very likely to have been exposed to tuberculosis. And I think it makes perfect sense to be screening them."
Both Mandalakas' study and Long's commentary recommend the screening begin swiftly after an international adoptee arrives in his or her new home.
And both recommended that the initial skin test be followed up three to six months later with another. That's because a test performed immediately after arrival might not detect an infection that occurred shortly before a child left an overseas orphanage.
Children who test positive should be put on a nine month course of antibiotics, Mandalakas said. She also suggested orphanages involved in international adoptions should test for tuberculosis among employees.
http://canadianpress.google.com/article/ALeqM5g_3TL6bspoGhwMS_sb1_nbv6KAeQ
SUMMARY OF TB VACCINES CURRENTLY UNDER DEVELOPMENT
Although it is generally acknowledged that a new safe and effective TB vaccine is needed, it may not be universally accepted, by all countries, that replacing the current bacille Calmette-Guérin (BCG) vaccine is in fact necessary or easily accomplished. However, with an integrated approach, for example using the current BCG vaccine in a prime––boost strategy, vaccination can make a major contribution to the elimination of TB
Comprehensive preclinical testing of vaccine products is needed to provide supportive evidence for the safety, immunogenicity, and potential effectiveness of the vaccine as well as for estimating vaccine dose and immunization schedules for clinical testing in human populations. Preclinical and nonclinical tests for regulatory purposes include the development of critical product tests such as potency/stability assays, toxicology assays relevant to vaccines, and safety assays. A recent publication on the development of live TB vaccines discusses useful methods for characterizing live TB vaccine products using good manufacturing practices (GMP). Also, Rowland et al. have described a number of tests that have been used to characterize the three major types of TB vaccine candidates: adjuvanted subunit vaccines, genetically modified vaccines, and vectored vaccines
The evaluation of new TB vaccine candidates in clinical trials will depend on several factors, including: (1) characteristics of the target study population, (2) the incidence of TB within the population, and (3) the incidence of atypical mycobacteria and of other infectious diseases such as HIV and malaria in the region where the clinical trial is being conducted. New preventive or therapeutic TB vaccines will need to be studied in several different clinical settings and in different populations, such as those who are "TB naïïve"(prior to infection), those with latent TB infection ("sensitized"), and those who have TB disease. In developing countries, key issues will include informed consent and access to immunization by the target population, as well as other risk/benefit and ethical issues.
Currently no immunologic correlate or surrogate marker for protection against TB infection or TB disease has been defined. Therefore safety and immunogenicity studies will need to provide data that allow researchers to make a reasonable decision based on the best science for moving forward into the next stage of clinical vaccine development within the shortest time frame possible (see http://www.fda.gov/oc/gcp/). Feasibility studies of new TB vaccines will need to address: (1) the choice of comparative controls for evaluating safety and efficacy, (2) determination of vaccine dose, (3) assessment of vaccine-induced human immune responses, (4) enrollment eligibility, particularly for persons previously infected with M. tuberculosis, and (5) retention of clinical trial materials for future studies
http://medicine.plosjournals.org/perlserv/?request=get_document&doi=10.1371/journal.pmed.0040252&
Comprehensive preclinical testing of vaccine products is needed to provide supportive evidence for the safety, immunogenicity, and potential effectiveness of the vaccine as well as for estimating vaccine dose and immunization schedules for clinical testing in human populations. Preclinical and nonclinical tests for regulatory purposes include the development of critical product tests such as potency/stability assays, toxicology assays relevant to vaccines, and safety assays. A recent publication on the development of live TB vaccines discusses useful methods for characterizing live TB vaccine products using good manufacturing practices (GMP). Also, Rowland et al. have described a number of tests that have been used to characterize the three major types of TB vaccine candidates: adjuvanted subunit vaccines, genetically modified vaccines, and vectored vaccines
The evaluation of new TB vaccine candidates in clinical trials will depend on several factors, including: (1) characteristics of the target study population, (2) the incidence of TB within the population, and (3) the incidence of atypical mycobacteria and of other infectious diseases such as HIV and malaria in the region where the clinical trial is being conducted. New preventive or therapeutic TB vaccines will need to be studied in several different clinical settings and in different populations, such as those who are "TB naïïve"(prior to infection), those with latent TB infection ("sensitized"), and those who have TB disease. In developing countries, key issues will include informed consent and access to immunization by the target population, as well as other risk/benefit and ethical issues.
Currently no immunologic correlate or surrogate marker for protection against TB infection or TB disease has been defined. Therefore safety and immunogenicity studies will need to provide data that allow researchers to make a reasonable decision based on the best science for moving forward into the next stage of clinical vaccine development within the shortest time frame possible (see http://www.fda.gov/oc/gcp/). Feasibility studies of new TB vaccines will need to address: (1) the choice of comparative controls for evaluating safety and efficacy, (2) determination of vaccine dose, (3) assessment of vaccine-induced human immune responses, (4) enrollment eligibility, particularly for persons previously infected with M. tuberculosis, and (5) retention of clinical trial materials for future studies
http://medicine.plosjournals.org/perlserv/?request=get_document&doi=10.1371/journal.pmed.0040252&
COST TO THE PUBLIC OF AN EPIDEMIC
The United Nations (UN) has called for international cooperation and surveillance among nation-members, to boost global health security against new diseases emerging at an unprecedented rate in an increasingly interconnected world, often with the ability to cross borders rapidly.
The report set out the WHO strategic action plan to respond to a pandemic. It also drew attention to the need for stronger health systems and for continued vigilance in managing the risks and consequences of the international spread of polio and the newly emerging strain of extensively drug-resistant tuberculosis (XDR-TB).
It noted that since 1967, at least 39 new pathogens have been identified, including HIV, the deadly haemorrhagic Ebola and Marburg fevers, and Severe Acute Respiratory Syndrome (SARS), which emerged in China in 2003 and spread rapidly as far as Canada, infecting more than 8,000 people, over 800 of them fatally, before it was brought under control.
Other centuries-old threats, such as pandemic influenza, malaria and tuberculosis, continue to pose a threat to health through a combination of mutation, rising resistance to anti microbial medicines and weak health systems. New threats have also emerged, linked to potential terrorist attacks, chemical incidents and radio-nuclear accidents, it added.
It showed how and why diseases are increasingly threatening global public health security, citing the high and rapid mobility of people as one factor. Airlines now carry more than two billion passengers a year, enabling people and the diseases that travel with them to pass from one country to another in a matter of hours.
The potential health and economic impact was seen in 2003 with SARS, which cost Asian countries an estimated $60 billion of gross expenditure and business losses.
http://allafrica.com/stories/200708290723.html
The report set out the WHO strategic action plan to respond to a pandemic. It also drew attention to the need for stronger health systems and for continued vigilance in managing the risks and consequences of the international spread of polio and the newly emerging strain of extensively drug-resistant tuberculosis (XDR-TB).
It noted that since 1967, at least 39 new pathogens have been identified, including HIV, the deadly haemorrhagic Ebola and Marburg fevers, and Severe Acute Respiratory Syndrome (SARS), which emerged in China in 2003 and spread rapidly as far as Canada, infecting more than 8,000 people, over 800 of them fatally, before it was brought under control.
Other centuries-old threats, such as pandemic influenza, malaria and tuberculosis, continue to pose a threat to health through a combination of mutation, rising resistance to anti microbial medicines and weak health systems. New threats have also emerged, linked to potential terrorist attacks, chemical incidents and radio-nuclear accidents, it added.
It showed how and why diseases are increasingly threatening global public health security, citing the high and rapid mobility of people as one factor. Airlines now carry more than two billion passengers a year, enabling people and the diseases that travel with them to pass from one country to another in a matter of hours.
The potential health and economic impact was seen in 2003 with SARS, which cost Asian countries an estimated $60 billion of gross expenditure and business losses.
http://allafrica.com/stories/200708290723.html
CDC TO PROVIDE AIRPORTS WITH TB PATIENT LIST SOON
STAY HOME: Health authorities said on Tuesday they had notified 1,100 TB patients that they are subject to travel restrictions to prevent the spread of the disease A new system to prevent travelers in the "open," or infectious phase of tuberculosis (TB) from boarding international flights more than eight hours long will go online next month, a Centers for Disease Control (CDC) official said yesterday.
The rules are even more stringent for patients infected with the rarer and more serious forms of TB, multidrug-resistant tuberculosis (MDR) and extensively drug-resistant tuberculosis (XDR).
"People in the infectious phase of MDR or XDR will not be allowed on any flights at all for the safety of other passengers," CDC Deputy Director Chou Chih-hao ( ? ? ?) said.
Health authorities had notified some 1,100 TB patients that they are subject to travel restrictions.
Chou said that 188 multi-drug-resistant TB patients and more than 900 other infectious TB patients have been placed under air travel restrictions.
http://www.taipeitimes.comhttp://www.taipeitimes.com/News/taiwan/archives/2007/08/30/2003376433
TB in Zambia and in Maryland
A friend of mine who lives in Zambia has adopted several of his brother’’s children over the last few years. They needed to be adopted because all his brothers had passed away from tuberculosis. They were all in their 30s and 40s, in the prime of their lives. Not one of them had to die. TB can be cured for as little as $20. We all learned about how serious it can be with the drug-resistant case of the newlywed groom in June of this year.
According to the [Department of Health and Mental Hygiene], Maryland had 283 cases in 2005. In Prince George’s County there were 57 cases. Though not alarming levels, they still need proper treatment.
In Africa, TB is the leading cause of death of those who are infected with HIV /AIDS, taking over two million lives a year.
It is time for Congress to act. The Stop TB Now Act of 2007 (HR 1567) would support efforts to treat the disease worldwide. It has passed a key House committee. Now it is time for our House Majority Leader, Rep. Steny Hoyer to make sure it becomes law by bringing it to a vote in September. By doing so, millions of mothers and fathers will get to enjoy the lives of their children
http://www.gazette.net/stories/083007/prinlet163336_32363.shtml
According to the [Department of Health and Mental Hygiene], Maryland had 283 cases in 2005. In Prince George’s County there were 57 cases. Though not alarming levels, they still need proper treatment.
In Africa, TB is the leading cause of death of those who are infected with HIV /AIDS, taking over two million lives a year.
It is time for Congress to act. The Stop TB Now Act of 2007 (HR 1567) would support efforts to treat the disease worldwide. It has passed a key House committee. Now it is time for our House Majority Leader, Rep. Steny Hoyer to make sure it becomes law by bringing it to a vote in September. By doing so, millions of mothers and fathers will get to enjoy the lives of their children
http://www.gazette.net/stories/083007/prinlet163336_32363.shtml
Wednesday, 5 September 2007
FROM ABKHAZIA
ABKHAZIA INSTTUTE FOR SOCIAL & ECONOMIC RESEARCH
Worldwide Emergence of Extensively Drug-resistant Tuberculosis
Written by Ramaz Mitaishvili
Saturday, 01 September 2007
Abstract Mycobacterium tuberculosis strains that are resistant to an increasing number of second-line drugs used to treat multidrug-resistant tuberculosis (MDR TB) are becoming a threat to public health worldwide. We surveyed the Network of Supranational Reference Laboratories for M. tuberculosis isolates that were resistant to second-line anti-TB drugs during 2000––2004. We defined extensively drug-resistant TB (XDR TB) as MDR TB with further resistance to >3 of the 6 classes of second-line drugs. Of 23 eligible laboratories, 14 (61%) contributed data on 17,690 isolates, which reflected drug susceptibility results from 48 countries. Of 3,520 (19.9%) MDR TB isolates, 347 (9.9%) met criteria for XDR TB. Further investigation of population-based trends and expanded efforts to prevent drug resistance and effectively treat patients with MDR TB are crucial for protection of public health and control of TB.
Multidrug-resistant tuberculosis (MDR TB) has been documented in nearly 90 countries and regions worldwide; 424,203 cases of MDR TB were estimated to have occurred in 2004, which is 4.3% of all new and previously treated TB cases. Treatment for MDR TB patients requires use of second-line drugs for >24 months. These drugs are more costly, toxic, and less effective than first-line drugs used for routine treatment of TB. As with other diseases, resistance to TB drugs results primarily from nonadherence by patients, incorrect drug prescribing by providers, poor quality drugs, or erratic supply of drugs. To facilitate treatment of MDR TB in resource-limited countries, where most TB cases occur, the World Health Organization (WHO) and its partners developed the Green Light Committee, which helps ensure proper use of second-line drugs, to prevent further drug resistance. Nonetheless, the Green Light Committee encountered numerous anecdotal reports of MDR TB cases with resistance to most second-line drugs. Once a strain has developed resistance to second-line drugs, these new TB strains are even more difficult to treat with existing drugs. Untreated or inadequately treated patients are at increased risk of spreading their disease in the community, which could lead to outbreaks in vulnerable populations and widespread emergence of a lethal, costly epidemic of drug-resistant TB, reminiscent of the MDR TB outbreaks in the early 1990s. Therefore, to determine whether these anecdotal reports were isolated events, early evidence of an emerging epidemic, or the occurrence of virtually untreatable forms of drug-resistant TB that had not been described previously in different parts of the world, we characterized and quantified the frequency of second-line––drug resistance in several geographic regions.
Worldwide Emergence of Extensively Drug-resistant Tuberculosis
Written by Ramaz Mitaishvili
Saturday, 01 September 2007
Abstract Mycobacterium tuberculosis strains that are resistant to an increasing number of second-line drugs used to treat multidrug-resistant tuberculosis (MDR TB) are becoming a threat to public health worldwide. We surveyed the Network of Supranational Reference Laboratories for M. tuberculosis isolates that were resistant to second-line anti-TB drugs during 2000––2004. We defined extensively drug-resistant TB (XDR TB) as MDR TB with further resistance to >3 of the 6 classes of second-line drugs. Of 23 eligible laboratories, 14 (61%) contributed data on 17,690 isolates, which reflected drug susceptibility results from 48 countries. Of 3,520 (19.9%) MDR TB isolates, 347 (9.9%) met criteria for XDR TB. Further investigation of population-based trends and expanded efforts to prevent drug resistance and effectively treat patients with MDR TB are crucial for protection of public health and control of TB.
Multidrug-resistant tuberculosis (MDR TB) has been documented in nearly 90 countries and regions worldwide; 424,203 cases of MDR TB were estimated to have occurred in 2004, which is 4.3% of all new and previously treated TB cases. Treatment for MDR TB patients requires use of second-line drugs for >24 months. These drugs are more costly, toxic, and less effective than first-line drugs used for routine treatment of TB. As with other diseases, resistance to TB drugs results primarily from nonadherence by patients, incorrect drug prescribing by providers, poor quality drugs, or erratic supply of drugs. To facilitate treatment of MDR TB in resource-limited countries, where most TB cases occur, the World Health Organization (WHO) and its partners developed the Green Light Committee, which helps ensure proper use of second-line drugs, to prevent further drug resistance. Nonetheless, the Green Light Committee encountered numerous anecdotal reports of MDR TB cases with resistance to most second-line drugs. Once a strain has developed resistance to second-line drugs, these new TB strains are even more difficult to treat with existing drugs. Untreated or inadequately treated patients are at increased risk of spreading their disease in the community, which could lead to outbreaks in vulnerable populations and widespread emergence of a lethal, costly epidemic of drug-resistant TB, reminiscent of the MDR TB outbreaks in the early 1990s. Therefore, to determine whether these anecdotal reports were isolated events, early evidence of an emerging epidemic, or the occurrence of virtually untreatable forms of drug-resistant TB that had not been described previously in different parts of the world, we characterized and quantified the frequency of second-line––drug resistance in several geographic regions.
CONTINUING EPIDEMIC PROPORTIONS
Independent Online, Capetown
Sept 1, 1977
Huge rise in TB reported in E Cape
The Nelson Mandela Bay metropolitan area is grappling with an increasing number of tuberculosis cases, with about 250 new patients being admitted to Livingstone and Dora Nginza hospitals each month. In addition to this, over 200 new multi-drug resistant (MDR) TB patients are transported from throughout the province to the Jose Pearson Hospital in Bethelsdorp each month, according to Port Elizabeth Hospital Complex chief executive officer Lulamile JamJam. TB control specialists have appealed to businesses to prioritise TB in the workplace and put in place programmes to strengthen the community response to TB, The Herald Online reported on Friday. According to the national TB crisis management plan, the Eastern Cape is ranked second in the country in numbers of patients referred to hospitals and the low cure rate recorded. KwaZulu-Natal has the most TB cases, followed by Eastern Cape and then Western Cape and Gauteng. In an effort to create awareness, national experts on tuberculosis control met business leaders and councillors in Nelson Mandela Bay during a TB breakfast briefing this week. The theme of the function, which was initiated by the health department, the US Agency International Development and the University Research Corporation, was managing TB in the community and workplace. In spite of the challenge posed by TB, speakers were optimistic and emphasised that the war could be won. The disease should not be the country's leading cause of mortality, but victory needed a concerted effort. "TB is a critical public health problem, but it is also a social issue. We will not get this epidemic under control without strengthening our health systems," said Dr Lindiwe Mvusi, head of the national TB control programme. - Sapa
Sept 1, 1977
Huge rise in TB reported in E Cape
The Nelson Mandela Bay metropolitan area is grappling with an increasing number of tuberculosis cases, with about 250 new patients being admitted to Livingstone and Dora Nginza hospitals each month. In addition to this, over 200 new multi-drug resistant (MDR) TB patients are transported from throughout the province to the Jose Pearson Hospital in Bethelsdorp each month, according to Port Elizabeth Hospital Complex chief executive officer Lulamile JamJam. TB control specialists have appealed to businesses to prioritise TB in the workplace and put in place programmes to strengthen the community response to TB, The Herald Online reported on Friday. According to the national TB crisis management plan, the Eastern Cape is ranked second in the country in numbers of patients referred to hospitals and the low cure rate recorded. KwaZulu-Natal has the most TB cases, followed by Eastern Cape and then Western Cape and Gauteng. In an effort to create awareness, national experts on tuberculosis control met business leaders and councillors in Nelson Mandela Bay during a TB breakfast briefing this week. The theme of the function, which was initiated by the health department, the US Agency International Development and the University Research Corporation, was managing TB in the community and workplace. In spite of the challenge posed by TB, speakers were optimistic and emphasised that the war could be won. The disease should not be the country's leading cause of mortality, but victory needed a concerted effort. "TB is a critical public health problem, but it is also a social issue. We will not get this epidemic under control without strengthening our health systems," said Dr Lindiwe Mvusi, head of the national TB control programme. - Sapa
Subscribe to:
Posts (Atom)