30 March 2010
U.S. Strategy Expands Tuberculosis Treatment, Control
Goals include faster TB detection, more HIV tests, stronger health systems
By Cheryl PellerinScience Writer
Washington ― On World Tuberculosis Day, March 24, the United States released a five-year strategy for dealing with the ancient and relentless contagious lung disease that sickens 9 million people a year and kills nearly 5,000 every day in some of the world’s poorest nations.
The strategy, called for by the 2008 Lantos-Hyde Leadership Act Against AIDS, TB and Malaria, details the government’s plans from 2009 to 2014 to address the global public health threat of TB, including multidrug-resistant TB (MDR-TB) and extensively drug-resistant TB (XDR-TB), forms of the disease that threaten to undermine recent progress in controlling TB.
“As part of the President’s Global Health Initiative we are accelerating our programs to control TB,” Dr. Rajiv Shah, administrator of the U.S. Agency for International Development (USAID), said in a video March 24 as he released the strategy.
“Working with our many partners,” he said, “we believe it will be possible to halve the number of TB cases and deaths by 2015. In doing so, 14 million lives could be saved.” The plan lays the groundwork for detecting and treating TB in 2.6 million people and 57,200 MDR patients.
“This is our blueprint for expanded treatment and control over the next five years,” Shah said. “We will work in close partnerships with host nations to implement this strategy.”
DEADLY CONTAGION
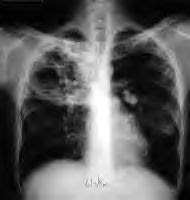
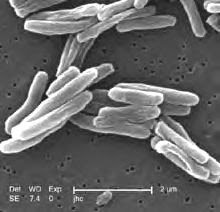
One-third of the planet’s population is infected with TB, which can be deadly if it becomes active in the body and is left untreated. The immune system can keep TB bacteria under control after a person becomes infected, but bacteria can become active when something — a medical condition such as HIV, for example — reduces a person’s immunity.
People in almost every country are infected with TB, but 22 countries account for 80 percent of the TB cases. The countries, in order, are India, China, Indonesia, Nigeria, South Africa, Bangladesh, Ethiopia, Pakistan, Philippines, Democratic Republic of Congo, Russia, Vietnam, Kenya, Brazil, Tanzania, Uganda, Zimbabwe, Thailand, Mozambique, Burma, Cambodia and Afghanistan.
TB is treated with a six- to nine-month course of “first-line” (most effective) drugs that cost less than $20. If patients do not complete the drug course or are treated improperly, they can develop MDR-TB. These patients must be treated with more expensive, less effective second-line drugs for 18 to 24 months.
If patients do not complete this course or are treated with the wrong drugs, they can develop XDR-TB, whose bacteria strains are resistant to all TB drugs. Fewer than 30 percent of XDR-TB patients who are otherwise healthy and whose immune systems are not compromised can be cured. More than half of those with XDR-TB die within five years of diagnosis.
http://www.america.gov/st/scitech-english/2010/March/20100330131534lcnirellep0.721081.html
WHAT'S NEW IN TUBERCULOSIS
Thursday, 8 April 2010
Subscribe to:
Post Comments (Atom)



No comments:
Post a Comment